5 solutions to improve practice management, patient experience
Let’s face it, the expectations of your patients have changed. Today, patients want to be able to communicate directly with their care providers, they want to be seen quickly for wellness visits, and they want the option to meet with doctors remotely from their own home. With these evolving expectations from patients come new challenges for care providers and healthcare organizations.
Recent data shows that total appointment wait times have increased by 1-4 minutes in the past year and are up to 7 minutes longer than they were pre-pandemic.1 The need for efficient, high-quality care is rising, but many healthcare organizations across the country are battling high burnout rates2 and turnover while trying to deliver the best care possible. But the risks of failing to improve the patient experience are high, even when care providers are faced with other serious headwinds. Sacrificing the quality of the patient experience -- and patient attrition --ultimately means sacrificing the potential growth of your business.
So, how can your healthcare organization keep up?
You can start by leveraging relevant services that help your practice deliver effective care to patients and help create the efficiency you need to focus on larger business goals. We’ve curated a brief list of five athenahealth services that are designed to not only help you strengthen patient relationships, but provide accessible care, drive efficiency, and take control of your revenue. Ready to dive in?
Strengthen relationships and empower patients with patient engagement services
38% of medical practices say no-shows are their biggest challenge with appointments.3 For many, there’s a real struggle to keep patients engaged in their wellness and care, battling issues like care gaps, outdated technology, and patient attrition.
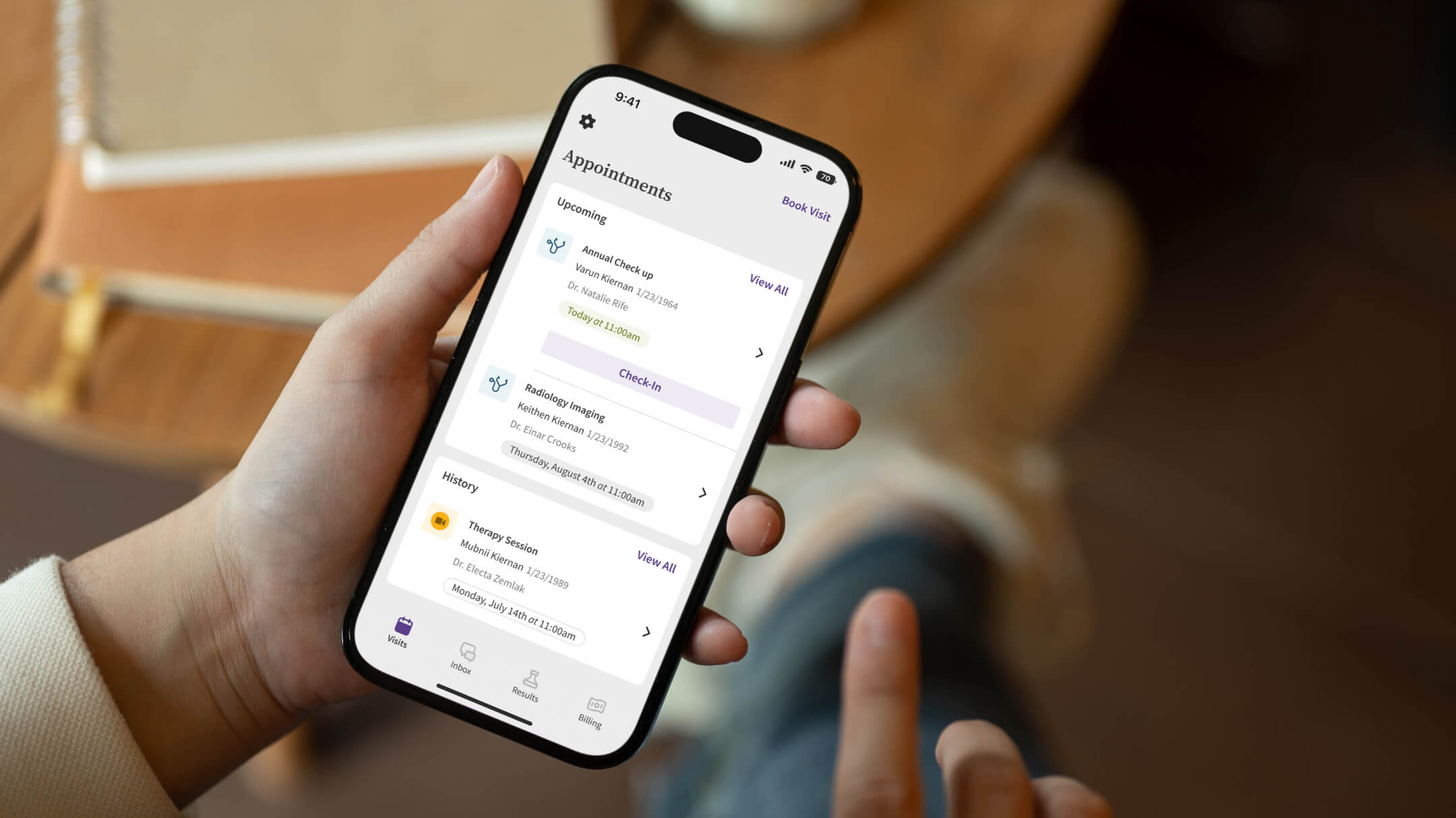
Strong patient-practice relationships start by meeting patients where they are. 26% of patients are willing to switch to a new provider for high-quality digital services.4 Your patients want to be able to schedule wellness visits quickly and easily, and message directly with their care provider when they have questions. Using the right patient portal, you can empower patients with self-serve tools that expand access to necessary health information and their care team. With a mobile-friendly app, patients can schedule, make payments, receive care via telehealth, and more, all from their phone.
What if a patient wants to reach out to you directly? Frequent, clear communication is essential to providing high-quality care and keeping your practice thriving. Patient engagement tools make staying connected easy through outreach messages and automated reminders that help close care gaps and collect more revenue for your healthcare organization.
Save time with interoperability and data exchange services
Having to spend valuable time searching through countless documents and digital repositories to locate critical patient information is an efficiency-killer for care providers and staff. It also contributes to high burnout rates. Almost half (49%) of physicians express feeling burnout from work every week or more.5
To help combat this, you can start by reducing documentation time during patient encounters using an EHR that prioritizes data exchange and interoperability. With the right EHR, you can exchange integrated clinical data with external healthcare IT entities and other partners to get the critical data you need to properly manage care for your patient population. What’s more, you can help reduce time spent on manual entry using helpful tools like best-practice templates, macros, accelerators, with patient records that proactively integrate data from a comprehensive network of care sites.
When choosing the right EHR for you, consider a solution that aggregates, maintains, and normalizes your clinical and payer data to deliver a single source of truth. This will have the long-term benefit of creating efficiency for your healthcare organization, allowing you to spend more one-on-one time with your patients, thereby improving the patient experience and instilling a sense of confidence and loyalty in your practice.
Gain control over your healthcare organization’s bottom line with revenue cycle solutions
Let’s face it: It’s getting harder for doctors and care providers to get paid, especially those who work in smaller organizations with only a handful of doctors. Denials rose to 11% of all claims last year, up nearly 8% from 2021.6 Payer takebacks, coupled with barriers to being paid what’s owed and on-time, are continuing to drive negative revenue cycle performance for many healthcare organizations. And failure to drive consistent revenue has often put doctors and care providers into survival mode, fighting to just keep their doors open.
By leveraging the right revenue cycle management (RCM) software and services, you can get paid faster, with less work, and at a lower cost. RCM solutions can help you maximize your financial performance and drive efficiency at every stage of your revenue cycle, from patient registration all the way to performance reporting. You can also help reduce A/R days and drive down the cost of collections by increasing automation, reducing redundancies, and fostering best practice workflows. And support that ensures that none of your claims are denied. One small, family-oriented practice was able to leverage medical billing services to not only increase revenue, but gain time back in the day to focus on higher value tasks and patient care.
And, as your organization evolves, your revenue cycle services can, too. With flexible and intuitive tech, you can scale RCM services to match your healthcare organization’s needs as your business grows and optimizes.
Expand access to care and grow your patient roster with telehealth services
Since the pandemic, we’ve seen a steady increase in telehealth services across healthcare organizations. In fact, there’s been a 23x rise in telehealth utilization since 2020 and $15.3 billion total in U.S. investments in digital tech in 2022.7 So, why is telehealth so popular?
Telehealth services allow you to provide more accessible care to patients who otherwise wouldn’t be able to make an in-office appointment. Elderly patients, patients with mobility issues, and patients with chronic illnesses are all groups who benefit greatly from providers that offer telehealth as an option to receive care. As a provider, you can expand access to care by using telehealth services to stay in touch with patients and provide the care they need. Telehealth services that offer automated patient outreach, group video conferencing, and integrated billing help to simplify and create efficiency for your organization. One medical center in New Mexico was even able to provide flexibility to patients so they could easily convert an in-person visit to a telehealth appointment, helping patients keep their appointments and filling care gaps along the way.
Telehealth allows you to meaningfully engage with patients and meet them wherever they are, but it also allows you to grow your patient roster and maintain schedule density. By leveraging telehealth services in addition to in-person care, your healthcare organization can grow to accommodate new patients while fitting more appointments in a day. And this helps ensure a steady flow of revenue for your practice.
Document more efficiently with voice-powered services
Many care providers say time spent documenting patient encounters is a huge challenge for their organization. Overall, physicians spend over 15 hours per week on paperwork and administrative tasks.8 For smaller practices in particular, the amount of time spent taking notes can be a huge burden, and it subtracts time that would otherwise be spent connecting directly with patients and fostering relationships.
Voice-to-text dictation may sound like a thing of the future, but it’s quickly becoming a highly used service among healthcare organizations looking to cut down on documentation time. powered services that drive efficiency. Using voice powered services, you can help reduce documentation time, boost productivity, and create new efficiencies during patient encounters. Some intuitive services can actually retrieve clinical information and allow you to complete meaningful clinical tasks hands-free, from either your desktop or mobile device. One independent pediatric practice used voice dictation services to move from closing only 55% of charts per day to closing 75%, reducing wait times and freeing up clinicians' time as well.
By integrating voice dictation services into your day-to-day, you can spend less patient time in front of a screen, and more time connecting one-to-one with your patient population.
Better patient care leads to better chances of growth and longevity for your healthcare organization. By leveraging tools and services available to you with the right EHR, you can improve the overall patient experience, create new efficiencies, expand your patient roster, and get paid faster.
Not sure where to start? We’re happy to help. Our suite of EHR, RCM, and patient engagement solutions help enable outstanding care for your practice, while maximizing revenue. Learn more about how you can optimize your practice’s performance using athenaOne.
More patient satisfaction resources
Continue exploring
MGMA, August 2023, DataDive Practice Operations; https://mgma.com/getkaiasset/ef6e357a-412b-41de-848f-a1b506b4261b/MGMA-PracticeOperations-DataReport-August2023-FINAL.pdf
2. AMA, Pandemic pushes U.S. doctor burnout to all-time high of 63%, Sep 2022, https://www.ama-assn.org/practice-management/physician-health/pandemic-pushes-us-doctor-burnout-all-time-high-63
3. MGMA, March 15, 2022, Stat Poll; https://www.mgma.com/mgma-stats/back-to-normal-or-new-normal-optimizing-appointments-is-the-key-to-your-revenue-cycle
4. Accenture, August 2020, How can leaders make recent digital health gains last?;
https://www.accenture.com/us-en/insights/health/leaders-make-recent-digital-health-gains-last;
IS50
5. athenahealth, 2022, Physician Sentiment Survey;
https://www.athenahealth.com/sites/default/files/media_docs/PSS2022.pdf; IS25
6. American Medical Association, Health Systems Plagued by Payer Takeback Schemes, Jan 2023
https://www.ama-assn.org/practice-management/prior-authorization/health-systems-plagued-payer-takeback-schemes-110000#:~:text=According%20to%20Crowe%2C%20payer%20takebacks,the%20retraction%20of%20previous%20payments.
7. Advisory Board, 2023, Understanding Your Customer: Physicians and Medical Groups; https://www.advisory.com/topics/physician/2023/06/understand-your-customer-physicians-and-medical-groups
8. Becker’s Hospital Review, The Hours 23 Physician Specialties Spend on Paperwork, Administration, April 2023;
https://www.beckershospitalreview.com/hospital-physician-relationships/the-hours-23-physician-specialties-spend-on-paperwork-administration.html#:~:text=Overall%2C%20physicians%20spend%2015.5%20hours,hours%20are%20on%20EHR%
20documentation.










