Expert insights on AI in healthcare, physician burnout, patient communication, and more from athenahealth’s 2025 Physician Sentiment Survey
Our 2024 Physician Sentiment Survey results showed widespread physician burnout and an alarming percentage of physicians who were considering leaving the field of medicine.1 In last year’s article, I speculated whether AI in healthcare could be the key to addressing physician burnout by reducing documentation and administrative burden. Now our results are in for the 2025 Physician Sentiment Survey (PSS), fielded by The Harris Poll, and confirm that artificial intelligence (AI) in healthcare may indeed be the key to addressing physician burnout.
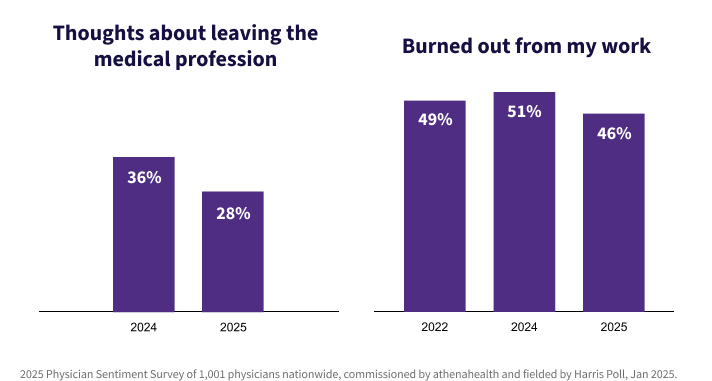
I’m happy to report that in 2025 there was a nearly 10 percent decrease in physician burnout since last year, and significantly fewer physicians are considering leaving the medical profession.2 And not just that, physicians in our survey are reporting that they are rediscovering the joy in medicine and their work.
What changed? The answer here is clear: Artificial intelligence in healthcare has rapidly evolved over the past 12 months and seems on track to transform the way physicians leverage technology in healthcare.
With that, I’m excited to share this new data showing how physician sentiment has evolved in the past year, which common pain points persist, and how healthcare technology has been rising to meet the needs of clinicians.
Positive changes in overall physician sentiment
While physician burnout is still an ongoing challenge in healthcare, we’re finally starting to see a change in the tides. Over two thirds (68%) of physicians in the 2025 PSS said that in the past year, they looked forward to coming to work each day at least once a week or more.3
Physicians are now more confident that healthcare is heading in the right direction, and that technology may finally be fulfilling its promise to help take on the work. This is a major shift in sentiment, and one that I hope to see carried forward into the future. While multiple factors might be driving the changes in sentiment, the results from this year’s PSS indicate that improvements in technology, especially the use of AI to address administrative burdens, are a main driver.4 For years EHRs were cited as one of the major contributors to physician burnout, so it stands to reason that as the technology improves, we’ll hopefully start to see sentiments improve as well.
Clinical documentation burden eased by use of AI in healthcare
In last year’s survey, physicians were optimistic but also quite skeptical with regards to AI, fearing that it would be yet another thing on their plate. The new results from the 2025 PSS shows that positive sentiment on AI from physicians has grown, along with increased optimism about coming to work.5
Ambient AI note generation has really blossomed in the last year, and more physicians are seeing the immediate benefits. Our survey responses showed that over two thirds (68%) of physicians who use AI in their practice said that in the past year, their use of AI to help generate clinical documentation increased.6 They also view the biggest potential benefits as helping improve clinical documentation (48%) and helping reduce administrative burden (46%).7
The explosion of ambient note generation seems to have shown physicians what is possible: AI taking on administrative burden and freeing up physician time.
It’s clear to me from our survey that our approach at athenahealth to focus first on reducing administrative burden is the right one – doctors enjoy being doctors when technology is not in their way. While we don’t want to jump to leveraging AI for every single human interaction right out of the gate, I definitely believe there are opportunities to improve the experience for everybody and not lose that human touch if we choose to do it in a thoughtful way – such as the use of AI in patient communications.
“Patient communication is one of the most important things as a physician that you can do, however that doesn’t mean it’s not overwhelming. In medicine, we seem to always go from one extreme to another—it’s time to find the happy medium.”
- Dr. Nele Jessel
Physicians still face growing pressure to keep up with patient communication
Patients during the pandemic learned to lean on the virtual world to keep up with care. While this is great for engagement, it also means that physicians are now expected to spend more time answering patient messages.
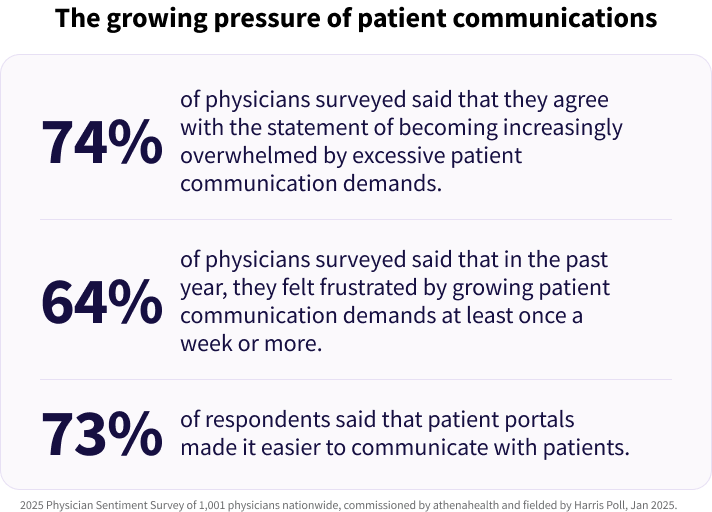
The 2025 PSS revealed that 74% of respondents agree that they’ve become increasingly overwhelmed by patient communication.8 In last year’s PSS, we found that 60% said they’re expected to be available all hours of the day, every day of the week.9 Based on our data, we’ve seen that patient communications are adding to physician administrative burden.
However, there’s a bit of a dichotomy here: 73% also agreed that patient portals have made it easier to communicate with patients.10 So, physicians are simultaneously grappling with frustrations around patient communication expectations, but don’t necessarily believe that patient communication tools are the problem.
The two aren’t mutually exclusive: engaging with patients is one of the most important things you can do as a physician. But that doesn’t mean it’s not overwhelming. In medicine, we seem to always go from one extreme to another—it's time to find the happy medium.
We must get smarter about how we leverage communications and put safeguards in place—for both physicians and patients—so there’s mutual understanding for what will and won’t get answered, and how soon the response will come. There's an opportunity to leverage artificial intelligence in this role, so simple inquiries can get answered by AI and more complex cases can be routed to physicians for a response or an appointment. Automated replies can be a big help in this instance, while still maintaining control from the physician about what lands in their inbox.
The challenge of data exchange and interoperability in healthcare
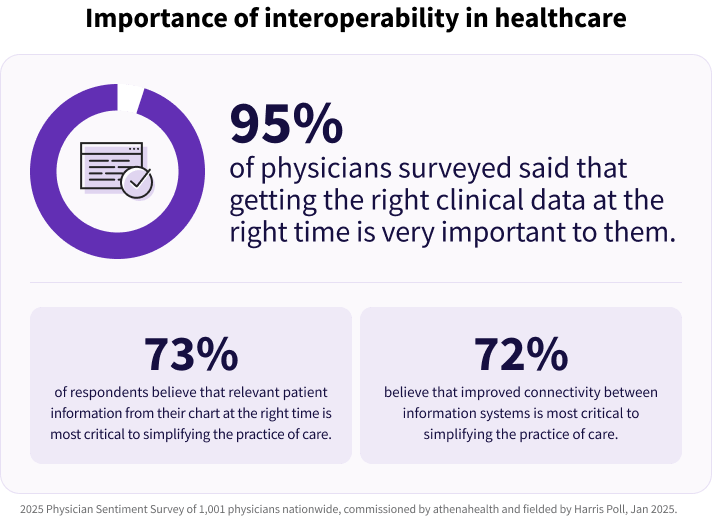
In this new survey, 95% of physicians said that getting the right clinical data at the right time is very important to them, and 73% believe that relevant patient information from their chart at the right time is the most critical factor in simplifying the practice of care.11 We can clearly see that improved connectivity between EHRs and information systems is not only vital to better patient care but making physicians’ lives easier overall – if we can effectively address the ongoing challenge of information overload while we continue to strive for better connectivity.
This is another opportunity where AI can help simplify the practice of care by alleviating the administrative burden: AI-powered data extraction, de-duplication and summarization can help filter through the noise and present only the most important, relevant information in a contextual manner, so it’s easily consumable.
So, where do we go from here?
We’re starting to see the promise of AI come to fruition, but there’s still more to come on how physicians will be able to leverage new developments of AI in healthcare. As our data shows, using AI to drive clinical efficiency and reduce administrative burden has high potential to save time and relieve stubborn challenges for clinicians.
But there’s still more to come on how physicians will be able to leverage new developments of AI in healthcare. I’m hopeful that physician burnout will continue to decrease with the measured and intentional implementation of AI, as long as we continue to balance these efficiencies with a focus on spending more time with patients and improving health outcomes. That is, after all, our end goal. Enabling clinicians to elevate the practice of medicine is truly what’s most important, and this just brings us one step closer.
More athenaInstitute resources
Continue exploring
- 2024 Physician Sentiment Survey of 1,003 physicians nationwide, commissioned by athenahealth and fielded by Harris Poll.
- 2025 Physician Sentiment Survey of 1,001 physicians nationwide, commissioned by athenahealth and fielded by Harris Poll, Jan 2025.
- 2025 Physician Sentiment Survey
- 2025 Physician Sentiment Survey
- 2025 Physician Sentiment Survey
- 2025 Physician Sentiment Survey
- 2025 Physician Sentiment Survey
- 2025 Physician Sentiment Survey
- 2024 Physician Sentiment Survey
- 2025 Physician Sentiment Survey
- 2025 Physician Sentiment Survey









