In the age of high deductibles, elective surgery tops the list of billing challenges. Informing patients of their out-of-pocket costs — when the numbers can be eye-popping — is a job for the most skilled members of a billing team.
Or is it?
Georgia Hand Shoulder Elbow, an Atlanta-area orthopedic group, came up with an innovative way to deploy front-office staff. “Our schedulers are our financial counselors," says Lynn Wolff, the organization's CEO. “They're bound and determined that they're going to get every co-pay."
It's an approach that enterprise organizations could learn from and scale. In an ongoing project, athenahealth researchers are examining key financial and operational metrics from across a national network of 99,000 providers and have identified the top 10 percent of performers. Georgia Hand Shoulder Elbow is one — with an enviable patient pay yield of 92 percent.
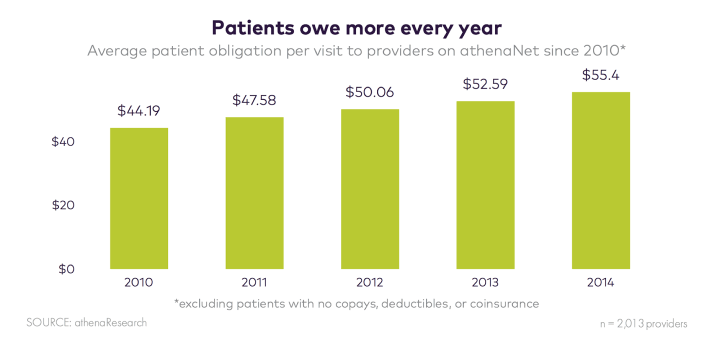
At medical organizations of all sizes, the art of building positive relationships with patients has been severely challenged by the growing demands of collections. The average obligation, for commercially insured patients, has increased by more than 20 percent over the past four years. That means front office staff frequently struggle to balance warm welcomes with requests for money.
At Georgia Hand Shoulder Elbow, that's where the surgery schedulers come in. On a daily basis, they serve as air traffic control, tracking every patient through pre-surgical testing to post-op, keeping an eye on operating room capacity and pulling from waitlists to fill cancellations. They're multi-tasking, problem-solving, calm-under-pressure communicators.
So they're perfectly placed to ask for payment on the spot, before a procedure can be scheduled, Wolff says.
In her practice, two surgery schedulers manage the scheduling and collecting process for three orthopedic surgeons each. When a physician recommends a patient for surgery, the patient is guided to a sub-waiting area while his paperwork is delivered to the surgery scheduler.
The scheduler reviews the planned procedure, the patient's insurance coverage and deductible, and the portion of that deductible that has been met. She then creates a spreadsheet of allowable costs for the relevant billing codes.
Then the patient joins the scheduler to review the form.
“It's a straightforward conversation," says Wolff. “The scheduler says, 'This is the procedure we plan to do, this is our charge, this is what your insurer will pay, and this is your deductible amount. And we need to collect that before we schedule the surgery.'"
Patients appreciate the clarity, even when they're taken aback by their own obligations, Wolff says. "If patients know their financial responsibility up front," agrees Owen Dahl, an independent practice management consultant, "they can make necessary arrangements. They know they are being cared for by a well-run, well-organized practice. That eases their mind and makes the whole process of care easier."
A protocol that empowers staff
The process works with the right people driving it. "Our schedulers challenge themselves and they get excited," says Wolff, to collect every payment due. And the team has been given the training and tools they need to get the job done. "What this practice has done is innovative and to be commended," says Dahl. "The schedulers are well prepared and understand that by discussing financial obligations, they are helping patients get the treatment they need. "
Our schedulers are our financial counselors. They're bound and determined that they're going to get every co-pay.
- Lynn Wolff, the organization's CEO CEO, Georgia Hand Shoulder Elbow
"Financial care for patients is as important as clinical care," says Sandra Wolfskill of the Healthcare Financial Management Association. "Price transparency is not about fees or schedules or charges. It is about telling patients what the price will be for them. For too long, we've made excuses about why we can't do that. But with the technology we have today, we can do that. If a patient's EHR and their insurance information is integrated with a pricing tool, we can help patients understand what they owe with compassion and empathy."
Gale Pryor is a senior writer with athenaInsight. Image credit: Darlene DeVita.












