Article
Specialists where there are no specialists
By Erin Graham | March 23, 2018
After an extended gap of a year and a half between visits, however, it was clear that Amanda hadn't been able to manage her hypertension on her own. “Her blood pressure was 240/130," says Mike Romagnoli, operations manager at the clinic. “In the past, we would have freaked out and called an ambulance."
Instead, the NPs managed Amanda's health crisis with medication and monitoring. Thanks to Project ECHO, they had just finished a series of teletraining sessions with a leading specialist on hypertension and were confident in their ability to stabilize the patient on their own.
A critical clinical connection
The University of New Mexico launched Project ECHO (Extension for Community Healthcare Outcomes) 14 years ago out to increase providers' access to specialty expertise – no matter where they are.
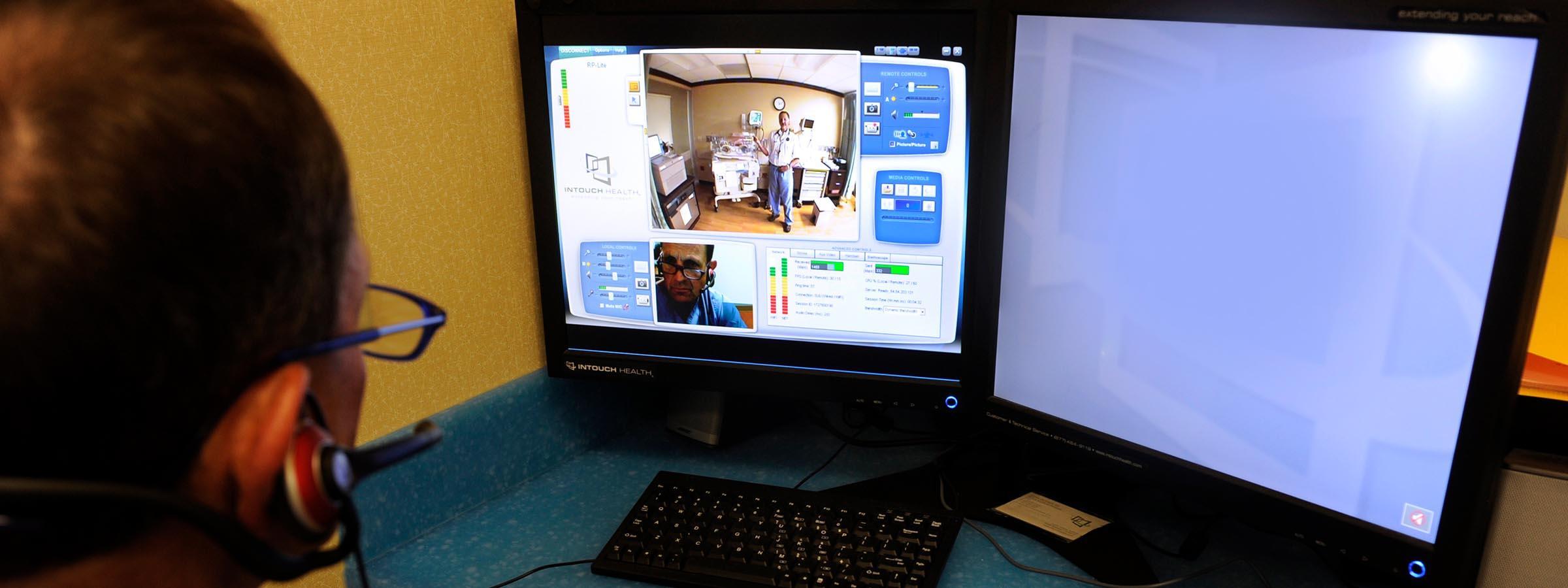
Via interactive videoconferencing, the program connects advanced specialists in teaching hospitals with nurse practitioners, physician assistants and community health workers in medically underserved areas. The volunteer specialists teach chronic disease management and conduct case-based learning to support clinical staff in remote communities with complex patient populations.
Sanjeev Arora, M.D., founded the program out of desperation. As a hepatologist at the University of New Mexico (UNM) Health Sciences Center in Albuquerque, he was frustrated at the difficulties rural patients with hepatitis C faced in getting the treatment they needed.
Arora's clinic was just one of two New Mexico that treated hepatitis C patients, who require yearlong weekly injections. “People would drive hundreds of miles to see me," Arora says. He estimates that out of the thousands of people who needed treatment, five percent or fewer were actually being treated.
Just 18 months after starting a remote hepatitis C training program, Arora saw his patients' wait time for appointments in Albuquerque fall from eight months to two weeks, as remote patients were able to get care closer to home.
Closing the specialist care gap
The Association of American Medical Colleges estimates a shortfall of 37,400 to 60,300 physician specialists by 2025. Specialists are scarce in rural locations, and when patients are referred to more populated areas, specialists there often aren't incentivized to treat uninsured, underinsured, or Medicaid patients. Even when referrals can be made, lack of transportation or work and childcare conflicts can prevent patients from making appointments.
So, bolstered by its ECHO Program training, the free clinic in Normal tries to do all it can onsite – everything from dispensing medications to managing severe hypertension like Amanda's. Besides, says Romagnoli, if they had sent Amanda to an emergency department, “they wouldn't have known her history like we do. And she would have returned with a medication list that isn't optimized for the outpatient setting."
Remote clinics aren't the only ones who benefit from the ECHO Program's virtual expertise. Nurse practitioner Emily Hendel directs Clinical Services at CommunityHealth in Chicago, a free clinic that provides care to more than 10,000 low-income, uninsured patients each year. For Hendel's team, location isn't the challenge, funding is. There simply isn't money for continuing education.
Along with Romagnoli's clinic and three others, Hendel's team participated in ECHO's weekly, one-hour hepatitis C trainings, 12 in all, facilitated by a University of Chicago specialist. During each of the virtual clinics, participants presented a case they were struggling with and talked about topics unique to the free clinic setting.
“We were all working with similar logistics that went beyond the shared challenge of limited specialist services, like how to get approval for treatment and medication for uninsured people," says Hendel.
For Romagnoli, ECHO's virtual clinics helped his team feel connected and confident, like any members of a community of practice and learning. “It's easy to feel like an island," he says. Now, “instead of waiting three to five months for an expert opinion, you have the knowledge base to address issues yourself."
Sharing expertise virtually
Since its founding, Project ECHO has expanded to 174 academic hubs focusing on 65 disease areas in 25 countries. And a 2011 study showed that the quality of hepatitis C care provided by Project ECHO-trained clinicians was equal to that of care provided by university-based specialists.
ECHO isn't the only program to use remote volunteers to help front-line primary care providers expand their skills. The MAVEN Project (Medical Alumni Volunteer Expert Network) recruits retired and semi-retired physician volunteers from medical school alumni associations across the country, along with physicians in practice.
“There is an increasing number of physicians looking to keep their identities as physicians who find it rewarding to bring resources to communities in need," says Lisa Levine, M.D., CEO of the MAVEN Project.
The service provides remote education sessions, one-on-one and group mentoring, direct-to-patient remote specialist appointments, and advisory consults. The demand for its mentoring services, in particular, is rising. “Clinics struggle with recruitment and retention of primary care providers, and this is a way for PCPs who may be new or looking for guidance to get structured support," says Levine.
Hub-and-spoke teaching models like ECHO and the MAVEN Project enable volunteer specialists to democratize their expertise – helping to get patients the right care, in the right place, at the right time, with the right knowledge – while freeing up their own calendars for more complex patients.
In Normal, Romagnoli estimates a 40 percent reduction in nephrology and cardiology referrals since joining Project ECHO, thanks to expanded in-house knowledge.
And in Chicago, Hendel says that her team has successfully treated 14 patients with hepatitis C to date, and that staff and her volunteers have completed other ECHO training sessions on treatment-resistant hypertension, high-risk women's health, and behavioral health.
'Sharpening the saw'
Asked if tele-training doesn't simply add work to already overtaxed PCPs, Arora says the opposite is true: For physicians, learning and managing complex medical problems with the support of specialist mentors is a form of "sharpening the saw."
Rachael Evans, M.D., chief medical officer at Henry J. Austin Health Center in New Jersey, agrees. “Think about how many hours are spent managing people in end-stage liver disease and how hard that is. It's not more complicated to do the front-end work than the back-end," says Evans, part of the team that originated Project ECHO at UNM.
For Romagnoli, the tele-training exponentially increases the quality of care being delivered locally. “It's definitely a commitment, but the benefits far outweigh the effort," he says. “You present one case, but you can take what you learn and apply it to 15 other patients."
Erin Graham is a frequent contributor to athenaInsight.






